Healthcare Claims Management Solutions Market Research, 2030
The global healthcare claims management solutions market size was valued at $12.7 billion in 2020, and is projected to reach $20.3 billion by 2030, growing at a CAGR of 4.7% from 2021 to 2030.
The healthcare claims management solutions is a process that includes optimization, bill filing, and updating & processing of medical claims related to the patients diagnosis, medications, and treatment. The healthcare claims management solutions are applied to ensure everything related to health insurance. There are different types of claim management software available in the market for patients to encourage loyalty by allowing quick and accurate process to resolves claims as fast as possible. Healthcare claims management software is used to streamline the medical claims process, which eases the relationship between providers and insurance companies and efficiently improves the patient payment lifecycle. Medical billing software, revenue cycle management software, and medical practice management software are some of the healthcare claim software that are available for customers and find application with payers, healthcare providers, and insurance providers.
Widely used software in the healthcare claims management solutions industry are Waystar, Kareo, TriZettoQNXT, NextGenHealthcare HER, eClinicalWorksRCM, anthenaCollector, Availity, and AdvancedMD. Athenahealth, Inc. provides cloud-based services for electronic health records, revenue cycle management & medical billing, patient engagement, care coordination, and population health management.

The key factors that drive the healthcare claims management solutions market growth include, rapid increase in aging population and subsequent rise in the number of chronic diseases. Moreover, there is a significant surge in demand for medical insurance among population to manage their out of pocket medical expenditure. Rise in medical insurance coverage among population and higher premium costs are some of the common healthcare claims management solutions market trends. Rapidly aging population and favorable demographics across the globe are expected to drive the demand for healthcare claim management solutions in the near future. Furthermore, increase in awareness for care provision and giving equal importance as that household spending leads to growth of the healthcare claims management solution market. Moreover, the involvement of government initiatives, such as the Ministry of Health & Family Welfare to improve the insurance cover of their citizens and adoption of cloud technology-related services offers a lucrative healthcare claims management solutions market opportunity. Improved focus on healthcare systems and advancement in technology for innovative treatments drive the growth of global healthcare claims management solutions market forecast.
On the basis of healthcare claims management solutions market analysis, the market is segmented into type, deployment mode, and geography. By type, the market is segmented into software, and services. On the basis of deployment mode, the healthcare claims management solutions market size is segmented into web-based, cloud-based mode, and on-premise mode. By geography, the market is segmented into North America, Europe, Asia-Pacific, and LAMEA.
Key players capturing healthcare claims management solutions market share are Oracle Corporation, ALLISCRIPTS HEALTHCARE SOLUTIONS, ATHENAHEALTH INC., COGNIZANT Technology Solution Corporation, Quest Diagnostics, McKesson Corporation, eClinicalWorks LLC, Optum, Inc., The SSI Group, Inc., and GE Healthcare.
By Type Segment Review
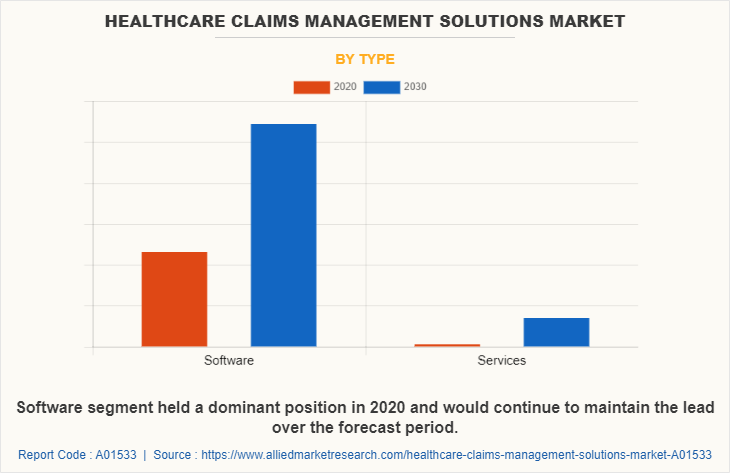
By type, the healthcare claims management solutions market size is segmented into software, and services. The software segment dominated the global healthcare claims management solutions market in 2020. This software provides an easy solution for all the tedious and time consuming claims management activities, such as eligibility crosschecking, benefit administration, premium billing, care management, claims processing, overpayment recovery, capitation, subrogation, customer service/contact management, fulfillment, reporting, and others. Use of software maximizes medical claims, billing functions, and capability allowing to generate bills for specific patient lists, and insurance carriers.
By Deployment Mode Segment Review
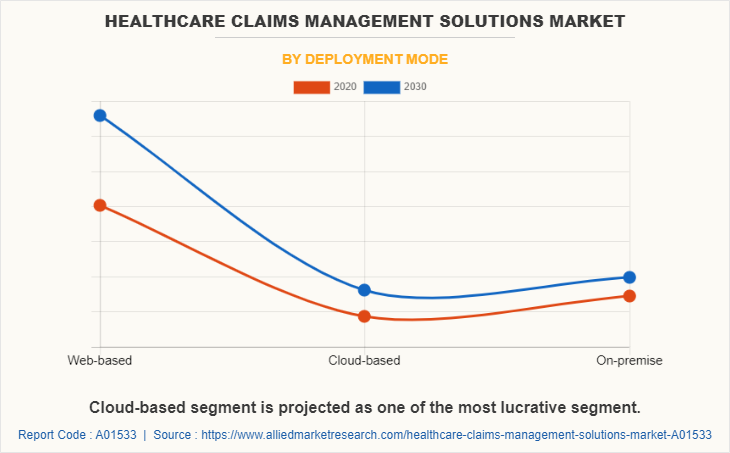
By deployment mode, the market is segmented into web-based mode, cloud-based mode, and on-site deployment mode. The web-based deployment mode dominated the global healthcare claims management solutions market in 2020. It provides flexibility and can be accessed anywhere and anytime, thus, the web-based deployment mode is highly adopted and preferred.
By Region Segment Review

By region, the market is segmented into North America, Europe, Asia-Pacific, and LAMEA. North America accounted for the largest market share in 2020 owing to well-established healthcare system in the region, rise in insurance coverage, and increase in the number of chronic diseases. However, Asia-Pacific is expected to emerge as the region with maximum growth potential due to focus of key players in emerging economies, improving healthcare infrastructure, and rising disposable income of middle class population in the region.
Key Benefits For Stakeholders
- This report provides a quantitative analysis of the healthcare claims management solutions industry, market segments, current trends, estimations, and dynamics of the healthcare claims management solutions market analysis from 2020 to 2030 to identify the prevailing healthcare claims management solutions market opportunities.
- The market research is offered along with information related to key drivers, restraints, and opportunities.
- Porter's five forces analysis highlights the potency of buyers and suppliers to enable stakeholders make profit-oriented business decisions and strengthen their supplier-buyer network.
- In-depth analysis of the healthcare claims management solutions market segmentation assists to determine the prevailing market opportunities.
- Major countries in each region are mapped according to their revenue contribution to the global market.
- Market player positioning facilitates benchmarking and provides a clear understanding of the present position of the market players.
- The report includes the analysis of the regional as well as global healthcare claims management solutions market trends, key players, market segments, application areas, and market growth strategies.
Healthcare Claims Management Solutions Market Report Highlights
| Aspects | Details |
| By Type |
|
| By Deployment Mode |
|
| By Region |
|
| Key Market Players | The SSI Groups Inc., Allscripts Healthcare Solutions, Inc., COGNIZANT TECHNOLOGY SOLUTIONS CORPORATION, McKesson Corporation, GE Healthcare, Quest Diagnostics, Oracle Corporation, eClinicalWorks LLC, Optum, Inc,, Athenahealth Inc. |
Analyst Review
In the global healthcare claims management solutions market, the software segment is the emerging with development and upgradation of the software, which largely contributes to the growth of the market. Software provide an easy solution for all the tedious and time consuming claims management activities, such as eligibility crosschecking, benefit administration, premium billing, care management, claims processing, overpayment recovery, capitation, subrogation, customer service/contact management, fulfillment, reporting, and more. The market is driven by increase in the aging population, rise in chronic diseases, and rise in population covered under various insurance schemes. The North America and Europe markets hold larger shares in the market due to increase in the use of software and services for the ease of claims processing and the presence of top insurance companies in these regions. Moreover, the well-established healthcare systems in these regions are one of the major reasons for the higher share of North America and Europe markets in the global healthcare claims management solutions market. Asia-Pacific is expected to witness market growth during forecast period as the region has the highest population of individuals suffering from chronic disorders, such as diabetes, coronary thrombosis, tuberculosis, and others and increase in the aging population.
Proactive government initiatives to improve insurance coverage among general population, and surge in use of cloud-based services are upcoming trends observed in the market
Healthcare claims management solutions are used across various healthcare facilities to simplify the process of billing, filling, updating, and processing of medical claims related to the diagnosis, treatment, and medication of patients.
North America is the largest regional market for Healthcare Claims Management Solutions
In 2020, the healthcare claims management solutions market size was valued at $12,690.3 million
Oracle Corporation, ALLSCRIPTS HEALTHCARE SOLUTIONS, INC., McKesson Corporation are some of the major players operating in healthcare claims management solutions market
Loading Table Of Content...



